Helping Sarah
Website Launched for Breast Cancer Australia

Statistics
Breast Cancer Australia has ongoing awareness and prevention campaigns including our 'One in 11 women will be diagnosed before the age of 75' message in conjunction with our daily 'pink ribbon' message. Awareness and prevention continues to be a driving factor in reducing the number of deaths from breast cancer. Early detection is the key to successful treatment.
Breast cancer is the most common of all cancers affecting Australian women and accounts for over 25% of all cancers diagnosed. The incidence of breast cancer in women has risen over 35% from 2004 to 2014. In Australia in 2014, a total of 16,614 women and 140 men were diagnosed with breast cancer.*
The mortality rate of Australians with breast cancer has largely stabilised from 2005 to 2015: in 2015 there were 2,967 deaths, compared to 2,729 in 2005, an increase of less than 10%.* Despite the significant loss of life, survival prospects continue to improve.
Early diagnosis is a key factor - over 98% of women will survive at least five years after diagnosis when the cancer is 10mm or less, virtually the same as women without breast cancer. This falls to 73% if the cancer has grown to 30mm or more, and 49% for other sized cancers. Equally, the 5-year survival rate for cancers which have not spread to the lymph nodes is 97%, compared to 80% when it has spread. §
Ongoing national research projects and the implementation of best practice at medical and diagnostic levels have signfiicantly increased the chances of survival today.
There is no known preventative treatment for breast cancer. However, there are now more rapid detection methods which can greatly reduce the time taken for accurate testing and detection and therefore treatment of a malignant tumour. This is crucial in reducing the chances of metastasis.
Detection
There are several different ways to detect breast cancer, starting with regular self examination.
Regular self examination
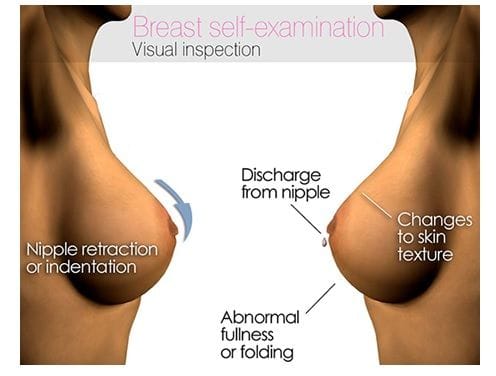
Look
Whilst standing in front of the mirror with shoulders back and hands on hips
- Check for changes in size, shape, and colour of both breasts
- Note if there is any dimpling, puckering, or bulging of skin
- Be aware of whether the nipple has changed position or if it has inverted
- Monitor for redness, soreness, rashness, or swelling
- It is also recommended to do this whilst the arms are raised in the air
Press
Apply minimal pressure with the thumb and forefinger to each nipple and check for discharge (milky, yellow fluid, or blood).
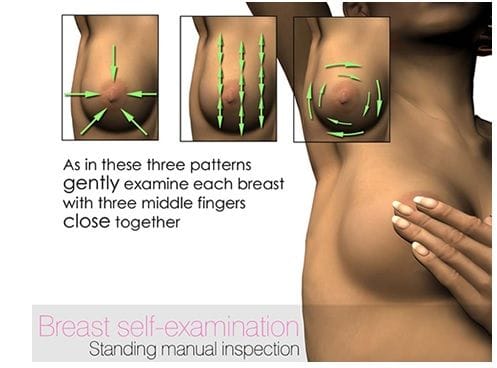
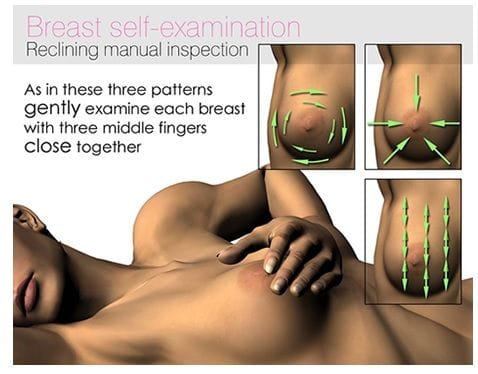
Feel
Feel your breast while lying down, sitting, standing, or in the shower.
- Use a method which you become familiar with and record your observations on a monthly basis
- When chekcing the left breast use your right hand (right breast, use your left hand) and work gently on the top layer and then a little firmer as you press deeper into the tissue with your middle three fingres feeling down to the ribcage
- Be sure to check all over your breast with a sequence you can remember. From the armpit to your cleavage, and from the top of the collarbone to the top of your stomach
- All the time, feeling for irregular lumps, lumpiness, or thickening, particularly in one breast only
Other than the presence of a physical lump, other symptoms include:
- Changes to the nipple
- Unusual discharge from the nipple
- Changes in the skin of the breast
- Lump, lumpiness, or thickening of the breast
- A change in the shape or size of a breast
- Unusual persistent pain
Things to consider:
- After your monthly regular self examination take into consideration any changes
- Some women prefer checking after their menstrual period as their breasts are less lumpy and less tender
- If there are any new unusual changes or persistent pain, see your doctor immediately
- Learn what is normal and seek medical advice if there are any issues which concern you
- It is important to mention if you are pregnant or going through menopause to your general practitioner
 |  |  |
If you find anything of concern, or have difficulty with self examination, you might consider medical examination with your local general practitioner. Your GP may then refer you for diagnostic mammography, which may lead to an ultrasound, fine needle biopsy, and/or core biopsy.
Between the ages of 50-74, free screening mammograms are conducted by BreastScreen Australia. Between 40-50 and after 75 they may be offered, depending on advice from your GP. Before the age of 40, mammograms are generally not effective, and other tests may be offered if there is cause for concern.
For information, and to book a BreastScreen appointment, call 13 20 50.
Causes
It is not possible to say what, exactly, causes breast cancer. However, research shows that some factors might increase the risk or chance of developing breast cancer.
Risk factors include:
- Being female. Over 99% of cases occur in women, although over 100 men are diagnosed each year as well.
- Getting older. This is the most common risk factor - slightly over 10% of cases occur in women aged under 50, over 60% of diagnoses occured in women aged between 50-75, the primary age group for screening, and the remaining 28% of cases were in women aged over 75.
- Having a family history. Between 5-10% of cases are thought to be due to mutations, most often in the BRCA1 and/or BRCA2 genes, which are inherited, and can lead to higher than normal rates of breast cancer in certain families.
- Previously being diagnosed with breast cancer. Unfortunately, the risk of developing a new cancer in either the same or other breast is 3-4 times more likely than if no previous cancer had existed. This is unrelated to recurrence of the original cancer.
There are other risk factors which seem to slightly increase a woman's risk of developing breast cancer:
- Starting menstruation, or periods, at a relatively early age (before 12 years), and/or starting menopause, or change of life, at a relatively late age (after 55 years)
- Not breast feeding - the more months spent breast feeding, the lower the risk of developing breast cancer
- Not having children, or having a first child after 35 years of age
- Taking combined Hormone Replacement Therapy (HT) after menopause, particularly when taken for 5 years or longer
- Drinking alcohol (more than 2 standard drinks a day)
- Taking the oral contraceptive pill - this appears to only increase the risk during the period of taking the pill, the risk goes back down after you stop taking it
- Having previously been diagnosed with lobular carcinoma in situ (LCIS) or atypical hyperplasia (AH)
Diet and exercise can help to prevent or reduce the risk of developing breast cancer. The following lifestyle habits are encouraged:
- Eating five or more portions a day of fruit and vegetables
- Eating regular servings of wholegrain cereal fibres and wheatbran
- Drinking two litres of water per day
- A minimum of 30 minutes aerobic exercise three times a week, or taking a brisk 30 minute walk five times a week
- Having a diet consisting of low-fat, high-fibre whole foods such as the leafy green vegetables, wholemeal products and pulses
- Calcium intake shoudl be around 1000-1200mg per day
- Red meat, full-fat dairy products, sugar, salt, and spicy foods should be limited
- Alcohol consumption should be taken in moderation
- Maintaining a healthy weight to height ratio ensures that your body is able to adequately deal with everyday activities
- Charred meats shoudl be particularly avoided, since they contain carcinogenic compounds
- Never smoking, or quitting if you have smoked, as many cancers are linked to smoking
- Limiting exposure to avoidable chemicals, such as those in cosmetics, food, and lawn, garden and chemical products
Treatments
Types of medical treatment include:
- Surgery
- Chemotherapy
- Radiation therapy
Myths Vs Facts
Here are five common myths about breast cancer.
Myth #1
An abnormality (lump) found in your breast means that you have breast cancer
Fact
An abnormality found in your breast does not necessarily mean that you have breast cancer. Approximately 80% of breast lumps are benign (non-cancerous). However, the likelihood of a lump being cancerous increases with age.
Some breast abnormalities that you may find are cysts (a build-up of fluid with the appearance of a circular lump), calcifications (small areas formed by a build-up of calcium salts situated in the breast tissue) or nipple discharge (often occuring in females taking certain medication such as oral contraceptive pills and may also occur due to touching, suckling, and/or aggravation from garments to the nipple area, or lactation).
Fear of finding an abnormality can cause women to skip regular self checks or visits to the doctor. However, early detection is the greatest type of prevention method.
Myth #2
Possessing a family history of breast cancer means that you will also develop breast cancer
Fact
Having a family history of breast cancer does not increase your risk of getting breask cancer. The increase is minimal at approximately 5-10%.
Additionally, many breast cancers occur by chance, with it less likely to be a genetic cause if you or your relative(s) were older (50 or over) when diagnosed. Immediate relatives, being a grandmother, mother, sister, or daughter, are the only individuals included in a person's family history for this purpose.
If you do have a family history of breast cancer, five years prior to the age of that person when their cancer was detected, you should begin to have mammograms.
Myth #3
Men cannot contract breast cancer
Fact
Even though men have fewer breast cells than women, they can still contract breast cancer. An estimated 1 in 1,800 men, compared with 1 in 11 women, will develop breast cancer in their lifetime.
Even though this figure is relatively small, men should have routine breast checks with their general practitioner.
Myth #4
Breast cancer is a readily transmitted disease
Fact
Breast cancer is not a contagious disease. You cannot contract it from simply being around an individual who has breast cancer.
Breast cancer is actually the result of an irregular increase of cell growth in the breast tissue causing a malignant (cancerous) lump to form.
Myth #5
Mammograms can cause breast cancer
Fact
Mammograms are a safe and reliable method of x-raying an individual's breasts, to aid in identifying any images inside that person's breast area, whether they are benign or malignant.
When a mammogram is performed, the radiation level used is at the lowest amount possible, meaning that it is not a cause of breast cancer, and does not cause a pre-existing breast cancer to spread.
* Data sourced from Australian Institute of Health and Welfare website https://www.aihw.gov.au/reports/cancer/acim-books/contents/acim-books
§ Data sourced from Australian Institute of Health and Welfare website https://www.aihw.gov.au/news-media/media-releases/2007/oct/breast-cancer-survival-very-high-with-early-detect


